Periodontal Therapy Timeline: Diagnosis, Treatment, and Maintenance
Periodontal Therapy Timelinee: Diagnosis, Treatment, and Maintenance
Periodontal disease affects millions of people worldwide, yet many don't realize they have it until significant damage has occurred. At Dr. Ahmed Nurein's practice in Malindi and Watamu, we've helped countless patients reverse gum disease and restore their oral health through comprehensive periodontal therapy.
This guide walks you through the complete timeline of periodontal treatment—from the moment you're diagnosed through active therapy and into long-term maintenance.
Understanding Periodontal Disease Progression
Before we discuss treatment, it's important to understand how periodontal disease develops:
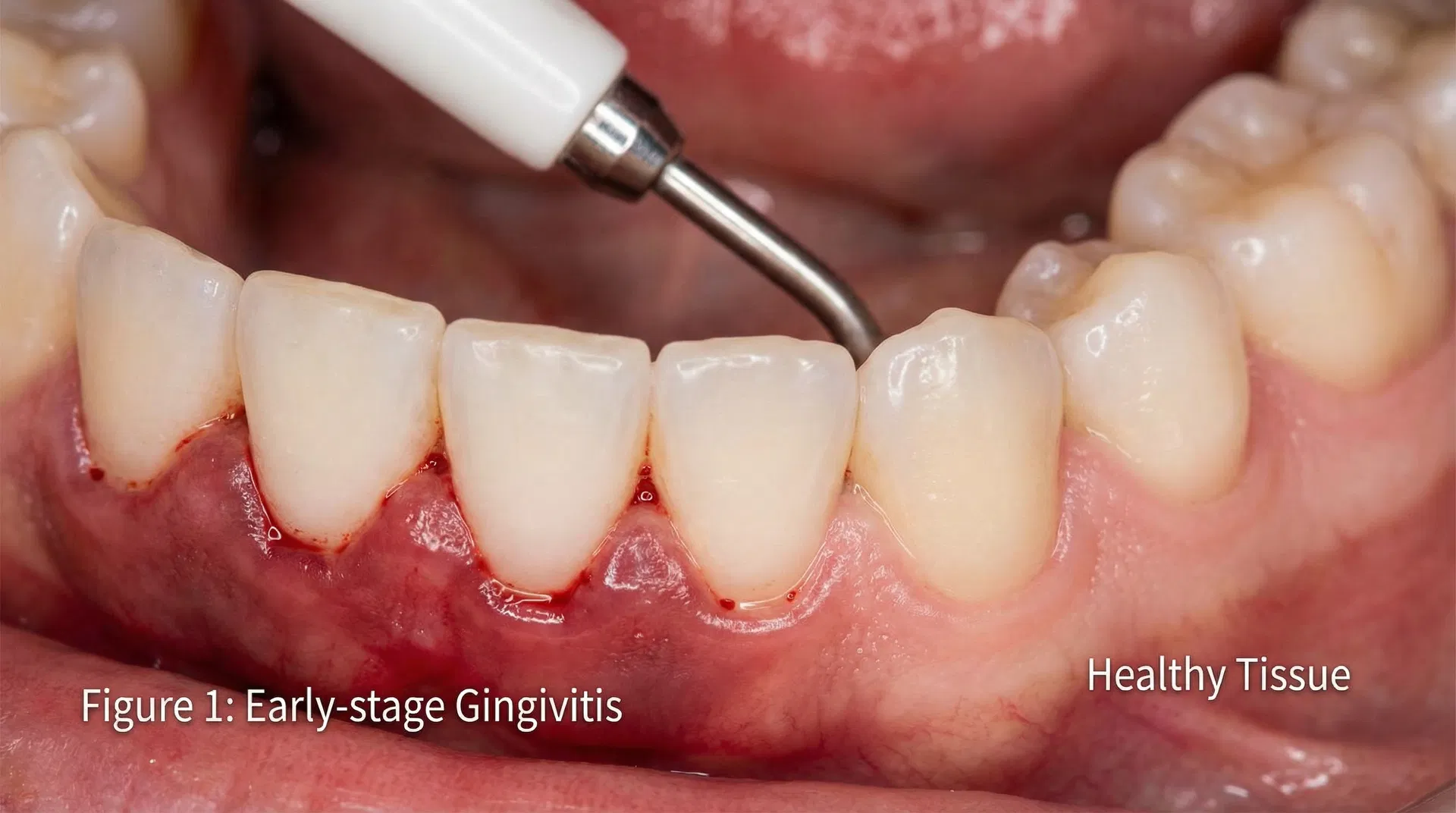
Stage 1: Gingivitis (Reversible)
Gingivitis is the earliest stage of gum disease:
- Red, swollen gums
- Bleeding when brushing or flossing
- Bad breath
- No bone loss yet
Good news: Gingivitis is completely reversible with improved oral hygiene and professional cleaning.
Stage 2: Early Periodontitis (Partially Reversible)
If gingivitis progresses, early periodontitis develops:
- Infection spreads below the gum line
- Slight bone loss begins (1-2mm)
- Periodontal pockets form (3-4mm)
- Gums may pull away from teeth
At this stage: Professional intervention can stop progression and partially reverse damage.
Stage 3: Moderate Periodontitis (Requires Treatment)
Without treatment, the disease advances:
- Significant bone loss (3-5mm)
- Deeper periodontal pockets (5-7mm)
- Increased mobility of teeth
- Possible tooth migration
- Visible gum recession
Treatment is essential: Scaling and root planing, and possibly surgical intervention.
Stage 4: Advanced Periodontitis (Severe)
In advanced cases:
- Severe bone loss (>5mm)
- Very deep pockets (>7mm)
- Teeth are loose and may be lost
- Significant aesthetic concerns
Treatment becomes complex: May require multiple surgical procedures or tooth extraction.
Phase 1: Diagnosis and Assessment (Week 1-2)
Your Initial Consultation
When you visit Dr. Ahmed Nurein with concerns about your gums, the first step is a comprehensive evaluation:
Clinical Examination:
- Visual inspection of gums for color, texture, and swelling
- Gentle probing to measure pocket depths (healthy pockets are 1-3mm)
- Assessment of tooth mobility
- Evaluation of gum recession
- Check for bleeding and suppuration
Diagnostic Imaging:
- Panoramic X-rays to assess bone levels
- Periapical X-rays for detailed tooth-by-tooth evaluation
- 3D cone beam CT scans in complex cases
Medical History Review:
- Discussion of risk factors (smoking, diabetes, stress)
- Current medications that may affect gum health
- Family history of gum disease
- Oral hygiene practices
The Periodontal Diagnosis
Based on this assessment, Dr. Nurein will classify your condition:
- Gingivitis: Inflammation without bone loss
- Stage I Periodontitis: 1-2mm bone loss
- Stage II Periodontitis: 3-5mm bone loss
- Stage III Periodontitis: >5mm bone loss with possible tooth mobility
- Stage IV Periodontitis: Advanced disease with severe bone loss
Treatment Planning
Dr. Nurein will discuss:
- Your specific diagnosis and severity
- Treatment options and recommendations
- Expected timeline and outcomes
- Cost and payment options
- Home care instructions to begin immediately
Phase 2: Non-Surgical Therapy (Week 3-8)
Scaling and Root Planing (Deep Cleaning)
For most patients with periodontitis, the first treatment is scaling and root planing (SRP), also called a "deep cleaning":
What Happens:
- Local anesthesia is administered to numb the area
- Ultrasonic and hand instruments remove plaque and tartar above and below the gum line
- Root surfaces are smoothed to remove bacterial toxins and promote healing
- Antimicrobial rinses may be used
Timeline:
- Usually completed in 2-4 appointments (one quadrant per visit)
- Each appointment lasts 45-60 minutes
- Appointments are spaced 1-2 weeks apart
What to Expect After:
- Mild discomfort for 24-48 hours
- Slight sensitivity to temperature
- Some bleeding for 24-48 hours
- Swelling may decrease over the next few days
Post-Treatment Care:
- Avoid hard, sticky, or hot foods for 24 hours
- Rinse gently with warm salt water after meals
- Take prescribed antibiotics as directed
- Use antimicrobial mouthwash
- Avoid smoking and alcohol
- Gentle brushing around treated areas
Antimicrobial Therapy
Dr. Nurein may recommend:
Local Antimicrobials:
- Chlorhexidine chips placed in deep pockets
- Antibiotic gels or powders
- Sustained-release medications
Systemic Antibiotics:
- Oral antibiotics (typically 7-10 days)
- Used in moderate to advanced cases
- Helps control bacterial infection
Evaluation Period (Week 6-8)
After scaling and root planing, you'll return for evaluation:
Assessment:
- Pocket depths are re-measured
- Bleeding is evaluated
- Healing is assessed
- Response to treatment is determined
Outcomes:
- Many patients show significant improvement
- Pockets may reduce by 1-3mm
- Bleeding typically stops
- Inflammation decreases
Next Steps:
- If healing is adequate: proceed to maintenance phase
- If inadequate response: consider surgical therapy
Phase 3: Surgical Therapy (If Needed) (Week 9-16)
If non-surgical therapy doesn't achieve adequate results, surgical intervention may be necessary.
Flap Surgery (Pocket Reduction Surgery)
Purpose:
- Access deep pockets for thorough cleaning
- Remove infected tissue
- Reshape bone
- Reduce pocket depth
Procedure:
- Local anesthesia is administered
- Small incisions are made in the gum
- Gum tissue is gently lifted (flapped)
- Tartar and diseased tissue are removed
- Bone is reshaped if necessary
- Tissue is repositioned and sutured
Recovery:
- 1-2 weeks for initial healing
- Sutures removed at 2 weeks
- Full healing takes 4-6 weeks
- Discomfort is managed with pain medication
Bone Grafting
In cases with significant bone loss, bone grafting may be recommended:
Purpose:
- Regenerate lost bone
- Create a more stable foundation
- Improve long-term prognosis
- Potentially save teeth
Materials Used:
- Autografts (your own bone)
- Allografts (donor bone)
- Xenografts (animal-derived bone)
- Synthetic bone substitutes
Timeline:
- 3-6 months for bone integration
- Requires careful maintenance
- May need additional procedures
Guided Tissue Regeneration (GTR)
GTR uses special membranes to:
- Guide bone and tissue growth
- Prevent epithelial cells from interfering with regeneration
- Improve healing outcomes
Procedure:
- Often combined with flap surgery
- Membranes are placed under the gum
- May be absorbable or non-absorbable
- Helps regenerate lost periodontal structures
Phase 4: Post-Surgical Healing (Week 17-24)
Immediate Post-Operative Care (Days 1-7)
Pain Management:
- Take prescribed pain medication as directed
- Over-the-counter pain relievers may help
- Pain typically peaks at 24-48 hours, then decreases
Swelling and Bruising:
- Swelling peaks at 48-72 hours
- Apply ice packs for 15 minutes on, 15 minutes off for first 24 hours
- Keep your head elevated
- Swelling typically resolves within 7-10 days
Oral Hygiene:
- Don't brush or floss near surgical sites for 2 weeks
- Rinse gently with warm salt water after meals
- Use antimicrobial mouthwash
- Avoid touching the surgical area
Diet:
- Stick to soft, cool foods
- Avoid hot, spicy, hard, or sticky foods
- No smoking or alcohol
- Don't use straws
Weeks 2-4 Recovery
Healing Progress:
- Sutures are removed at 2 weeks
- Swelling continues to decrease
- Pain becomes minimal
- You can gradually return to normal activities
Oral Care:
- Gentle brushing can resume around surgical areas
- Continue salt water rinses
- Use prescribed antimicrobial rinses
- Avoid aggressive flossing for 4-6 weeks
Weeks 4-12 Continued Healing
Tissue Maturation:
- Gum tissue continues to mature
- Bone begins to stabilize
- Pockets continue to shrink
- Inflammation resolves
Activity Level:
- Return to normal exercise
- Resume all normal activities
- Avoid very strenuous activity for 6 weeks
Phase 5: Evaluation and Transition to Maintenance (Month 3-4)
Post-Surgical Assessment
At 3-4 months post-surgery, Dr. Nurein will:
Clinical Evaluation:
- Measure pocket depths again
- Assess tissue healing
- Evaluate bone fill (if grafting was done)
- Check tooth mobility
- Assess overall periodontal health
Imaging:
- Take new X-rays to assess bone levels
- Compare to baseline images
- Evaluate graft integration (if applicable)
Outcomes:
- Most patients show significant improvement
- Pockets typically reduce by 2-4mm
- Bone loss may be partially reversed
- Teeth become more stable
Determining Success
Successful Treatment Indicators:
- Pocket depths reduced to 3mm or less
- No bleeding on probing
- Reduced tooth mobility
- Improved bone levels on X-rays
- Patient compliance with home care
If Results Are Inadequate:
- Additional procedures may be considered
- Tooth extraction may be necessary in severe cases
- Implant placement may be discussed
Phase 6: Long-Term Maintenance (Ongoing)
Periodontal Maintenance Therapy (PMT)
After active treatment, the most critical phase begins: maintenance. Without proper maintenance, periodontal disease will recur.
Frequency:
- Every 3 months (4 times per year) for most patients
- Every 2 months for high-risk patients
- Every 4-6 months for low-risk patients
What Happens at PMT Visits:
- Pocket depths are measured
- Bleeding is assessed
- Plaque and tartar are removed
- Root surfaces are smoothed
- Antimicrobial rinses are applied
- Oral hygiene is reinforced
Home Care Excellence
Maintenance success depends on your daily efforts:
Brushing:
- Twice daily for 2+ minutes
- Soft-bristled toothbrush
- 45-degree angle to gum line
- Gentle circular motions
- Electric toothbrushes are highly effective
Flossing:
- Daily flossing is non-negotiable
- Proper technique: gentle, curved around each tooth
- Water flossers are excellent alternatives
- Interdental brushes for larger spaces
Mouthwash:
- Antimicrobial rinse daily
- Chlorhexidine or essential oil formulations
- Use after brushing and flossing
Diet:
- Avoid sugary snacks and drinks
- Limit acidic beverages
- Eat gum-healthy foods (leafy greens, fatty fish, crunchy vegetables)
- Stay hydrated
Lifestyle Modifications
Smoking Cessation:
- Smoking is the #1 risk factor for recurrence
- Smokers have 3-6x higher risk of gum disease
- Quitting dramatically improves outcomes
- Ask Dr. Nurein for smoking cessation resources
Stress Management:
- Chronic stress suppresses immune function
- Practice relaxation techniques
- Exercise regularly
- Get adequate sleep (7-9 hours)
Diabetes Control:
- High blood sugar increases infection risk
- Work with your doctor for optimal control
- Inform Dr. Nurein of any changes
Medication Review:
- Some medications reduce saliva flow
- Discuss all medications with Dr. Nurein
- Consider alternatives if gum health is affected
Timeline Summary
| Phase | Duration | Key Activities |
|---|---|---|
| Diagnosis | Week 1-2 | Examination, X-rays, assessment, treatment planning |
| Non-Surgical Therapy | Week 3-8 | Scaling and root planing, antimicrobial therapy |
| Evaluation | Week 6-8 | Re-assessment, decision on surgical therapy |
| Surgical Therapy (if needed) | Week 9-16 | Flap surgery, bone grafting, tissue regeneration |
| Post-Surgical Healing | Week 17-24 | Recovery, suture removal, tissue maturation |
| Evaluation | Month 3-4 | Assessment of treatment outcomes |
| Maintenance | Ongoing | Quarterly professional cleanings and home care |
Periodontal Therapy and Dental Implants
If periodontal disease has resulted in tooth loss, dental implants offer an excellent solution. However:
Important Considerations:
- Gum disease must be treated and controlled before implant placement
- Implants require the same excellent home care as natural teeth
- Peri-implantitis (gum disease around implants) can occur if maintenance is neglected
- Regular professional visits are essential
Dr. Nurein can discuss implant options during your maintenance visits if tooth loss has occurred.
Your Periodontal Health Action Plan
This Week:
- Schedule a consultation with Dr. Ahmed Nurein
- Discuss your gum health concerns
- Receive a professional diagnosis
This Month:
- Begin recommended treatment
- Improve your home care routine
- Start smoking cessation (if applicable)
Ongoing:
- Attend all scheduled appointments
- Maintain excellent home care
- Attend quarterly maintenance visits
- Monitor your gum health
Conclusion
Periodontal disease is treatable. With Dr. Ahmed Nurein's expertise and your commitment to maintenance, you can achieve and maintain excellent gum health for life.
Remember: Periodontal health is the foundation of your entire smile. Invest in treatment today, and enjoy the benefits for decades to come.
Ready to restore your gum health? Schedule a consultation with Dr. Ahmed Nurein at:
- Malindi: +254 719 666 664 | [email protected]
- Watamu: +254 710 911 999 | [email protected]
- WhatsApp: +254 740 580 088
Dr. Ahmed Nurein is a periodontist and dental implant specialist with extensive experience in treating all stages of periodontal disease. Visit us at Star Specialist Hospital in Malindi or Watamu Reef Clinic in Watamu.
Share This Article
Help others discover valuable dental health information
About Dr. Ahmed Nurein
Dr. Ahmed Nurein is a periodontist and dental implant specialist with a BDS from the University of Nairobi and an MSc in Periodontology from Marmara University, Istanbul. He is a member of the Cambridge Academy of Dental Implantology and practices at Star Specialist Hospital in Malindi and Watamu Reef Clinic in Watamu, Kenya.
Schedule a consultation →Related Articles
Ready to Transform Your Smile?
Contact Dr. Ahmed Nurein today to discuss your dental implant options.
Book Consultation